Does CGM Help Reduce Post-Bariatric Hypoglycemia?
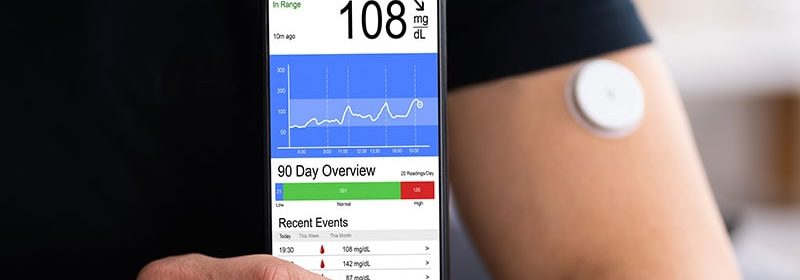
Continuous glucose monitors (CGMs) may help curb the severity of hypoglycemia after weight-loss operations and even other gastrointestinal procedures, according to recent findings from a small study published online in the journal Diabetes, Obesity, and Metabolism.
Hypoglycemia is a chronic and persistent complication common in patients following bariatric surgery, affecting as many as 30% of people who undergo a sleeve gastrectomy or Roux-en-Y gastric bypass.
The symptoms of hypoglycemia, including lightheadedness, heart palpitations, difficulty concentrating, and confusion, can mimic anxiety disorders, arrhythmia, and dumping syndrome.
If a postoperative patient experiences these symptoms within a few hours following a meal or exercising, “primary care doctors should consider the possibility that hypoglycemia may be a contributor,” said Mary-Elizabeth Patti, MD, director of the Hypoglycemia Clinic at the Joslin Diabetes Center in Boston and senior author of the new study.
“In fact, hypoglycemia is a possible diagnosis even among those who underwent [operations other than bariatric, including] fundoplication or other upper gastrointestinal or esophageal surgeries,” she said.
To understand how CGM could benefit patients, Patti and colleagues recruited 22 participants who had undergone bariatric surgery more than 8 years prior and had post-bariatric hypoglycemia. Their mean age was 51 years, 90% were women, 82% were diagnosed with level 3 hypoglycemia, and none had type 1 or 2 diabetes.
All participants experienced neuronal dysfunction with symptoms like fatigue, concentration difficulties, and confusion. More than 90% had received medical nutrition therapy for post-bariatric hypoglycemia in the past.
CGM data were collected in the 22 individuals in two sequential phases: masked (no access to sensor glucose or alarms) and unmasked (access to sensor glucose and alarms for low or rapidly declining sensor glucose). Twelve participants wore a CGM (Dexcom G4 device) for a total of 28 days, whereas 10 wore a CGM (the Dexcom G6 device) for a total of 20 days.
The team observed that the percentage of time when the participants’ blood glucose was below 70 mg/dL — the definition of hypoglycemia — was significantly lower during the unmasked phase.
Though CGM devices are not sensitive enough to serve as a diagnostic tool for hypoglycemia, “the alarms on CGM devices can provide some much-needed awareness,” Patti said. “After a detailed diagnosis, CGM devices can be a helpful tool to assess dietary patterns and make modifications that could reduce the severity of post-bariatric hypoglycemia.”
If a patient frequently experiences hypoglycemia, they may not sense when their glucose levels drop, also known as hypoglycemia unawareness, according to Patti. Studies have found that post-bariatric hypoglycemia remains underdiagnosed because most patients are asymptomatic.
“The use of CGM devices may improve safety in post-bariatric hypoglycemia, particularly for patients with hypoglycemia unawareness,” the researchers conclude.
Next Steps
Patients are more vulnerable to hypoglycemia after a sleeve gastrectomy or gastric bypass surgery because these procedures involve removing the pylorus. This valve plays a crucial role in only allowing small portions of food to enter the intestine and prevents sudden spikes in blood glucose.
Without the pylorus, large amounts of food directly enter the intestine and soon result in large amounts of glucose getting absorbed, according to Sriram Machineni, MD, an associate professor of medicine at the Albert Einstein College of Medicine In New York City, who was not affiliated with the study.
“The pancreas then goes into overdrive and produces a lot of insulin, which continues reducing sugar levels,” Machineni said. “That is what causes hypoglycemia.”
Patti and her team are next working on research using CGM-derived data to investigate how different types of meals, physical activities, and other factors could influence glucose metabolism patterns in patients with hypoglycemia.
The study was funded by Dexcom, a manufacturer of continuous glucose monitoring systems. Mary Elizabeth Patti reports receiving grant funding from the Diabetes Research Center.
Diabetes Obes Metab. Published online April 12, 2023. Abstract
Anuradha Varanasi is a freelance science journalist based in Mumbai, India. She has an MA in Science Journalism from Columbia University in New York City. You can follow her on Twitter @AnuradhaVaranas
For more Medscape Diabetes and Endocrinology news, follow us on Twitter and Facebook
Source: Read Full Article