Esophageal Varices

By Jeyashree Sundaram (MBA)
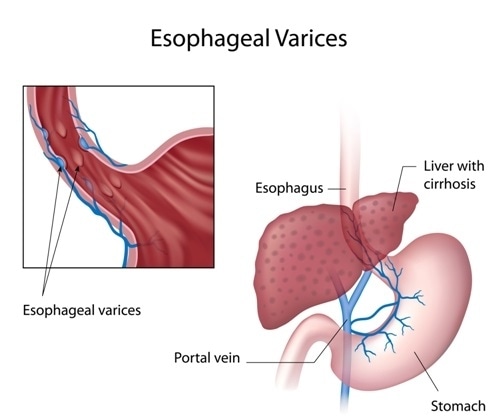
Veins that have become enlarged in the tube that interconnects the throat and stomach, the esophagus, are called esophageal varices. Those who are affected with severe liver disease will be particularly prone to developing esophageal varices.
Esophageal varices are developed either by the scar tissue of liver or a clot that blocks the regular blood flow towards the liver. These blockages causes blood to flow in the smaller blood vessels, which are not built to transmit large amount of blood. This can lead to life-threatening bleeding as a result of a leak of the blood flow and rupture at the vessels. Esophageal varices diagnosis should be performed, if a patient is affected with long-term liver diseases such as jaundice, ascites, or palmar erythema, etc.
Esophageal Varices Grading
Grading of esophageal varices helps in predicting the severity of bleeding risk and patient’s treatment route. They are best investigated using endoscopy. Esophageal varices develop from smaller sizes to larger sizes at roughly a rate of 8% each year. Esophageal varices development from small to large depends on various factors such as alcoholic cirrhosis, presence of red wheals (similar to the whip marks on the surface of a smaller vein), decompensated cirrhosis, and the hepatic vein pressure gradient. Esophageal varices develop whenever the hepatic vein pressure gradient is greater than 10 mm Hg. Large varices containing red wheals are at higher risk of rupture. Based on the size, the esophageal varices are classified as follows.
- Grade 1: Esophageal varices appear to be straight and small in size. Here, the varices extend just above the levels of mucus.
- Grade 2: Esophageal varices get enlarged and twisted and occupy less than one-third of the inside space of esophagus.
- Grade 3: Esophageal varices get enlarged and coiled and occupy more than one-third of the inside space of esophagus.
Causes
The liver plays a crucial role in blood detoxification and the portal veins are responsible for managing blood flow into the liver. Liver diseases will result in reduced blood flow rate through the liver, but an increased pressure in the portal veins. The additional load of blood in the portal veins forces it into nearby smaller blood vessels, causing esophageal varices.
The following conditions lead to esophageal varices development:
- Severe liver scarring (cirrhosis): Liver cirrhosis is the most common cause of esophageal varices. It is the condition where the healthy liver tissues are damaged and replaced by scar tissues. Chronic alcohol consumption is the main reason for liver cirrhosis. Overcoming alcohol addiction helps in preventing liver cirrhosis, which in turn prevents esophageal varices.
- Splenic vein thrombosis: Splenic vein thrombosis is an uncommon phenomenon of variceal bleeding. The esophageal varices develop as a result of portal hypertension caused by splenic vein thrombosis. This condition occurs when the blood flow through the splenic vein gets blocked or flows to the liver through short gastric veins.
- Budd-Chiari syndrome: Budd–Chiari syndrome is a very uncommon symptom of hepatic vein thrombosis, which leads to esophageal varices. In this condition, the flow of blood through hepatic veins (the vein that carries blood from liver to the inferior vena cava of heart) becomes blocked, subsequently resulting in hepatic vein thrombosis and esophageal varices.
- Portal hypertension: It is a condition in which there is an abnormal increase in portal vein blood pressure. This sudden increase in portal vein blood pressure occurs as a result of block in the vein that carries blood through the liver. It may also occur due to thrombosis. Portal hypertension may lead to swelling of portal veins, causing portal vein bleeding (esophageal varices).
Symptoms
Initially, symptoms of bleeding esophageal varices are not identified due to portal hypertension. Symptoms include severe bleeding in varices accompanied by vigorous hematemesis, leading to dizziness and loss of consciousness.
Lesser bleeding from varices may cause the patient to swallow the blood instead of vomiting. This often results in stool that contains blood becoming either a red or tarry-black color. The following are the symptoms of esophageal varices which occur due to cirrhosis and are accompanied by the symptoms associated with other liver diseases:
- Sensation of vomiting and noticing an indicative quantity of blood in the vomit
- Lightheadedness (sensation of dizziness or fainting sensation)
- Unconsciousness
- Jaundice (pale yellow discoloration in eyes and skin)
- Ascitic fluid enhancement (accumulation of abdominal fluid)
Prognosis
Bleeding is the most severe complication for esophageal varices. Patients undergoing treatment for esophageal varices at initial stages will experience recurrent bleeding within one to two years post-treatment. The condition can be fatal if there is massive blood loss due to esophageal varices bleeding.
Without hospitalization, esophageal varices bleeding cannot be controlled. It is a life-threatening emergency. At least 50% of patients identified with bleeding esophageal varices at initial stages are at risk of an increase in bleeding later on. This condition can be avoided by proper medication and endoscopy.
Transjugular intrahepatic portosystemic shunt treatment is suggested to prevent esophageal varices bleeding, but it may result in complexities in patients suffering from other liver diseases. Liver transplant may be a choice for patients suffering from liver cirrhosis and esophageal varices.
Sources
- www.lahey.org/…/Esophageal_Varices.aspx
- www.mayoclinic.org/…/ovc-20206457
- https://my.clevelandclinic.org/health/articles/esophageal-varices
- www.hepatitisc.uw.edu/…/all
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4976684/
Further Reading
- All Esophageal Varices Content
- Treatment for Esophageal Varices
- Preventing Esophageal Varices
Last Updated: Feb 26, 2019
Source: Read Full Article