online coupons clarinex
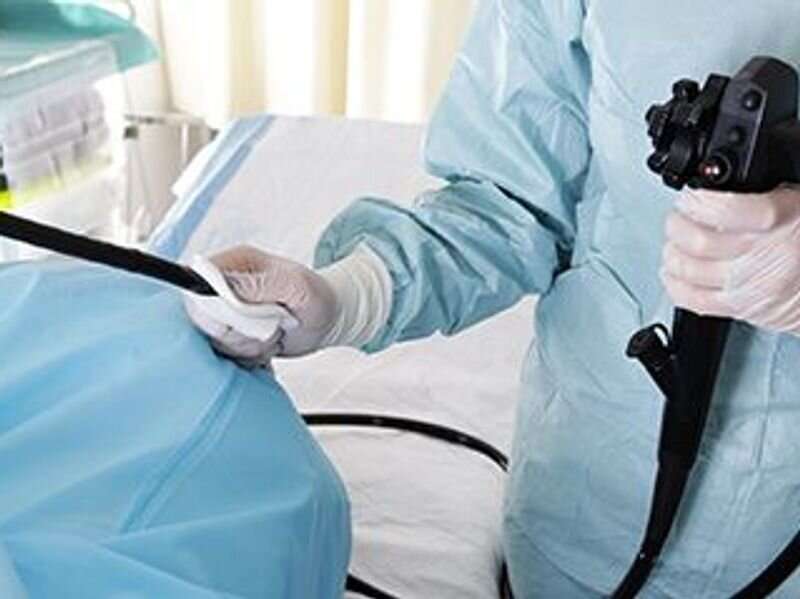
Among an average-risk population, follow-up colonoscopy (FU-CY) rates are low after a positive noninvasive stool-based screening test (SBT) for colorectal cancer, according to a study published online Jan. 18 in JAMA Network Open.
Jeff T. Mohl, doseage for cymbalta Ph.D., from the American Medical Group Association in Alexandria, Virginia, and colleagues conducted a mixed-methods study including a retrospective analysis of deidentified administrative claims and electronic health records data between June 1, 2015, and June 30, 2021, as well as interviews with clinicians from five health care organizations to assess FU-CY rates after a positive SBT result. The cohort study included 32,769 individuals (mean age, 63.1 years).
The researchers found that the FU-CY rates were 43.3, 51.4, and 56.1 percent within 90, 180, and 360 days, respectively, of the positive SBT result. When interviewed, clinicians were uniformly surprised by the low FU-CY rates. There was variation observed in rates by race, ethnicity, insurance type, presence of comorbidities, and type of SBT used. The strongest positive association was seen with multitarget stool DNA use (hazard ratio, 1.63 relative to fecal immunochemical tests), and the strongest negative association was seen with the presence of comorbidities (hazard ratio, 0.64 for a Charlson Comorbidity Index >4 versus 0).
“At-home stool-based testing offers a useful tool to supplement routine colonoscopy and reach a wider patient population,” the authors write. “Nonetheless, it is important to emphasize that all positive SBTs must be followed by a timely colonoscopy to complete the screening paradigm.”
The study was funded by the Exact Sciences Corporation.
More information:
Jeff T. Mohl et al, Rates of Follow-up Colonoscopy After a Positive Stool-Based Screening Test Result for Colorectal Cancer Among Health Care Organizations in the US, 2017-2020, JAMA Network Open (2023). DOI: 10.1001/jamanetworkopen.2022.51384
Journal information:
JAMA Network Open
Source: Read Full Article